Angular cheilitis is a condition in which the folds of the skin at the corners of the lips become exaggerated and irritated due to the retention of moisture or loss of epithelium. This appears as redness and cracking of the skin at the angle of the mouth. It may arise from many different causes.
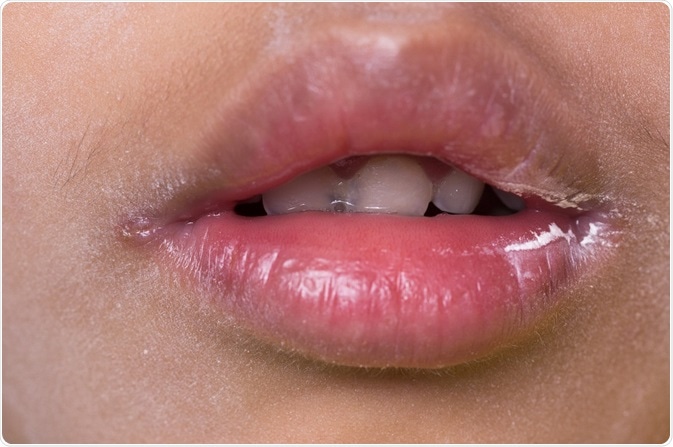
Credit: frank60/ Shutterstock.com
Common causes
- Angular cheilitis occurs most commonly in older people who suffer the loss of teeth. This leads to the upper lip overhanging the lower lip and thus making the corners of the mouth deeper, which results in the persistent presence of saliva and consequent irritation of the skin. This causes the skin to appear red and ulcerated. Oral candidiasis and secondary infection with Staphylococcus or Streptococcus may be also present.
- A naturally receding jawline also causes a higher risk of angular cheilitis.
- Poorly fitting dentures can increase the risk of infection in the moist crevices of the lip angles as may other causes of mechanical irritation.
- Angular cheilitis is also a known symptom of riboflavin deficiency but may also accompany iron, cobalamine and zinc deficiency
- Some skin conditions are also associated with angular cheilitis.
- Other causes may include:
- Immunodeficiency and general poor health, as in chemotherapy, diabetes or other acquired loss of normal immunity
- Treatment with certain drugs such as isotretinoin, antiretroviral drugs, antibiotics or systemic corticosteroids – these are also associated with oral candidiasis which is another risk factor for angular cheilitis
- Eczema because of excessively sensitive skin and increased susceptibility to infections
- Systemic conditions such as inflammatory bowel disease
- Habitual licking of the lips
- Dryness and peeling of the lip mucosa
- Genetic linkage with conditions such as trisomy 21 (Down syndrome)
Diagnosis
Immunosuppression should be asked for and looked for by testing if no obvious cause is evident. Allergic contact dermatitis is another commonly overlooked cause for angular cheilitis, and may be due to common flavoring agents, lip cosmetics such as sodium lauryl sulfate, and preservatives. Refractory angular cheilitis may be the only sign of malignancy. If the diagnosis is not unmistakable or there is evidence of any allergic condition underlying the perleche, a dermatologic consultation should be asked for.
Treatment
Angular cheilitis is sometimes a self-limited condition and then the treatment consists of symptomatic management. This includes the timely and frequent moisturization of the lips, with ointments, to avoid lip licking and minimize skin maceration.
When infection or eczema is present, topical antibiotics, antifungals, and steroids play a role. In oral candidiasis, which is almost always present in angular cheilitis, the best treatment is with oral and topical nystatin, or topical gentian violet, along with frequent cleaning and drying of the area.
In some cases, topical steroids are added to the use of anti-candidial ointments or lotions to reduce the inflammation. Desonide and hydrocortisone 1% are often recommended. If the candidiasis does not clear up with topical antifungal therapy, systemic fluconazole is prescribed in adults (with liver function monitoring). Systemic antibiotics may be needed, though rarely, if the infection does not subside with topical treatment.
Nutritional supplementation is necessary in case of iron or vitamin deficiency. In cases where the angles of the mouth are permanently overhung by the upper lips, filler material or implants may be used to restore firmness to the skin in this area and keep the angles of the mouth dry and clean. Surgery is useful to correct the redundant folds of skin at the angles of the mouth in edentulous patients. Elderly patients need prolonged barrier ointment use to prevent rapid relapses.
Faulty dentures should be adjusted for vertical height, and the patient shown how to clean them daily, in addition to the above measures for oral candidiasis.
In all patients, in between topical application of anti-infective agents, barrier ointments such as petrolatum or zinc oxide should be used to keep the area from becoming wet again, which hastens re-epithelialization.

0Comments